McKenzie exercises for sciatica may help some people reduce leg symptoms by using repeated movements that bring pain out of the leg and closer to the low back. That response is called centralization, and it is one of the core ideas behind the McKenzie Method. Not every case of sciatica responds well to extension-based exercise, so the goal is not to force through pain. The goal is to find movements that improve your symptom pattern, as explained in StatPearls.

Sciatica is a symptom, not a diagnosis by itself. It usually involves pain, tingling, numbness, or weakness that starts in the low back or buttock and travels down the leg. Common causes include a herniated disc or bony changes that irritate a nerve root, according to Mayo Clinic.
For many readers, the most useful takeaway is simple: start with the gentlest McKenzie exercise, watch how your leg symptoms respond, and only progress if the pain becomes more central, less intense, or easier to control. Official patient guidance from the NHS, Cleveland Clinic, and Mayo Clinic supports using movement carefully rather than staying completely inactive.
What are McKenzie exercises for sciatica?
McKenzie exercises are part of Mechanical Diagnosis and Therapy, a system that matches exercise direction to your symptom response. In low back pain with radiating symptoms, the method often emphasizes repeated end-range movements and self-management. Extension-based positions are common because many people with centralizing symptoms show an extension directional preference, though not everyone does, as described in StatPearls.
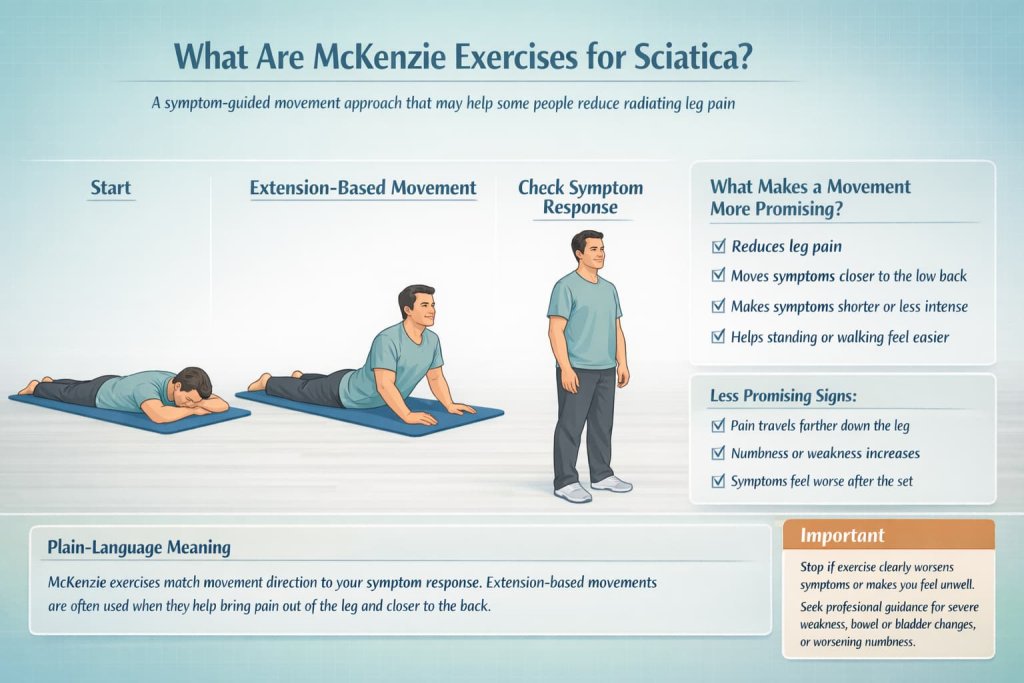
In plain language, that means a movement is more promising when it does one or more of these:
- reduces leg pain
- moves pain out of the calf or foot and closer to the back
- makes symptoms shorter or less intense after the set
- improves how easily you stand or walk afterward
A movement is less promising when it pushes symptoms farther down the leg, increases numbness or weakness, or leaves you feeling worse afterward. The NHS also advises stopping exercise if it causes pain or makes you unwell.
Are McKenzie exercises for sciatica actually effective?
The evidence is encouraging but not absolute. A 2025 systematic review available through PubMed Central found low-to-moderate certainty evidence that the McKenzie Method was superior to all other conservative interventions combined for short-term pain and intermediate-term disability in people with chronic low back pain with directional preference, though comparisons against manual therapy were much less impressive.

A randomized trial indexed by PubMed in people with MRI-confirmed sciatica due to lumbar disc herniation also directly compared a McKenzie intervention with guideline-based education, showing that the method has been studied specifically in sciatica populations rather than only in generic back pain groups.
That said, a 2018 review in JOSPT via PubMed found McKenzie is not clearly better than every other rehab option in all low back pain cases. The safest conclusion is that McKenzie exercises can be helpful, especially when your symptoms centralize with the chosen direction, but they are not a universal fix for every type of sciatica.
5 best McKenzie exercises for sciatica pain relief
These are the most practical McKenzie-style, extension-biased exercises commonly used in patient back-care progressions. South Tees Hospitals NHS Foundation Trust lists prone lying, and University Hospitals of North Midlands provides a clear prone-to-elbows-to-press-up progression with simple dosage guidance.
1. Prone Lying
How to do it:
- Lie on your stomach on a bed, mat, or firm surface.
- Let your arms rest by your sides and turn your head to one side.
- Take slow breaths and relax your back, hips, and legs.
- Stay here for 1 to 3 minutes.
- Repeat 3 to 4 times per day if it feels calming rather than aggravating.
Why it works:
Prone lying is the gentlest starting point in the McKenzie progression. It introduces your spine to extension without asking you to press up actively. For some people, this position alone can reduce leg pain or make the symptoms feel less spread out. South Tees Hospitals NHS Foundation Trust recommends prone lying for 1 to 2 minutes, and University Hospitals of North Midlands also uses a face-down starting position in its back exercise progression.
Muscles worked:
This is more of a positioning drill than a strengthening move. It places the lumbar spine in a mild extension posture while encouraging relaxation through the trunk and hip muscles.
Trainer Tip:
If lying flat is too intense, place one or two pillows under your stomach at first. University Hospitals of North Midlands specifically notes that pillows can make the starting position more comfortable.
2. Prone on Elbows
How to do it:
- Start lying on your stomach.
- Bring your elbows under your shoulders.
- Prop yourself up on your forearms.
- Keep your hips and pelvis heavy on the surface.
- Hold for 30 seconds to 3 minutes, depending on comfort.
- Repeat 3 to 4 times per day.
Why it works:
Prone on elbows increases extension a little more than basic prone lying. It is often the next step when the first position feels fine and your symptoms do not worsen. University Hospitals of North Midlands advises staying on the elbows while relaxing the back, hips, and legs, and notes that it should feel like a lower-back stretch without increasing back or leg pain.
Muscles worked:
Your shoulder stabilizers and upper trunk do a small amount of support work, but the main purpose is still symptom-guided spinal positioning rather than muscular overload.
Trainer Tip:
Watch the leg symptoms more than the back discomfort. A little local low-back pressure can be acceptable, but leg pain moving lower into the calf or foot is a warning sign to stop or back off. That symptom behavior fits the centralization approach described in StatPearls.
3. Prone Press-Up
How to do it:
- Lie on your stomach with your hands under your shoulders.
- Press through your hands to lift your chest.
- Keep your pelvis and hips on the floor.
- Straighten your elbows only as far as pain allows.
- Pause briefly at the top.
- Lower back down under control.
- Repeat 10 reps, up to 3 to 4 times per day.
Why it works:
This is the classic McKenzie extension-in-lying exercise. It increases lumbar extension more than the earlier stages and is often the main repeated movement used when extension clearly improves symptoms. University Hospitals of North Midlands recommends pressing the top half of the body up as far as pain permits, holding for about 2 seconds, and repeating 10 times.
Muscles worked:
Your arms and shoulders help you push up, while the lumbar area moves into extension. The goal is symptom change, not back-muscle fatigue.
Trainer Tip:
Do not squeeze your glutes hard or force the motion. Let your arms do most of the work so your low back can move without extra bracing.
4. Standing Back Extension
How to do it:
- Stand tall with your feet about hip-width apart.
- Place your hands on the back of your hips or pelvis.
- Gently lean backward from the waist.
- Keep the movement slow and controlled.
- Return to standing.
- Repeat 10 times.
Why it works:
Standing extension is a practical McKenzie option when you cannot get down to the floor during the day. It is commonly used as a maintenance movement between sets of prone work or during long periods of sitting. McKenzie literature frequently pairs repeated extension in standing or lying within its centralization framework, as outlined in StatPearls.
Muscles worked:
This movement lightly involves the spinal extensors and hip stabilizers, but again, the goal is directional symptom relief rather than strength training.
Trainer Tip:
This can be especially useful after long sitting because prolonged sitting is associated with disc-related aggravation risk and often makes some sciatica patterns feel worse, according to Mayo Clinic.
5. Repeated Extension Progression
How to do it:
- Begin with prone lying.
- Progress to prone on elbows if symptoms stay the same or improve.
- Move to prone press-ups only if the earlier stage is well tolerated.
- Perform 5 to 10 reps or short holds at the highest comfortable stage.
- Stop at the stage that gives the best symptom response.
Why it works:
Many people do better with a progression than with jumping straight into full press-ups. This staged sequence matches how South Tees Hospitals NHS Foundation Trust commonly presents lumbar extension exercises, starting with gentler positions and progressing only when tolerated.
Muscles worked:
The repeated extension progression is mainly about controlled spinal loading and symptom assessment. It is not intended as a bodybuilding-style exercise series.
Trainer Tip:
The best McKenzie exercise for sciatica is the one that centralizes your symptoms. That may be prone lying for one person and full press-ups for another.
How often should you do McKenzie exercises for sciatica?
McKenzie-style programs often use frequent, brief sessions rather than one long workout. StatPearls notes that patients commonly perform prescribed movements at home multiple times per day, and NHS hospital sheets often suggest 3 to 4 daily sessions for extension drills.
A simple starting plan:
- 1 to 2 exercises per session
- 5 to 10 reps for repeated movements
- 30 seconds to 3 minutes for hold positions
- 3 to 4 sessions per day
If symptoms improve, you can stay consistent for several days before gradually reducing frequency.
Before you start McKenzie exercises for sciatica
Try these exercises only if your symptoms are mild to moderate and you can move safely on your own. Get urgent medical help if you have bowel or bladder changes, saddle numbness, or severe or worsening leg weakness. Mayo Clinic notes that surgery is typically reserved for cases with severe weakness, bowel or bladder loss, or pain that does not improve with other treatment.
Quick safety checklist
- Stop if pain spreads farther down the leg.
- Stop if numbness or weakness clearly worsens.
- Move slowly and avoid bouncing.
- Use the gentlest version first.
- Progress only when the previous step feels manageable.
- Contact a clinician if symptoms are severe, confusing, or not improving.
What should you feel during these exercises?
You may feel:
- a mild stretch or pressure in the low back
- less intense leg symptoms afterward
- pain shifting upward toward the buttock or back
- easier standing or walking after the session
You should not ignore:
- symptoms spreading farther down the leg
- worsening numbness
- new weakness
- sharp pain that lingers after the set
Those changes suggest the movement may not be the right directional choice for you, which is consistent with the McKenzie symptom-response approach described in StatPearls.
Common mistakes when doing McKenzie exercises for sciatica
Pushing into worse leg pain
More pain is not always better. In McKenzie-based care, symptom location matters. Pain centralizing toward the spine is generally more favorable than pain moving farther down the leg, as explained in StatPearls.
Doing too many different exercises at once
If you mix flexion, extension, rotation, and stretching all in the same session, it becomes harder to know what is helping. Start simple and track your response.
Progressing too fast
Many people skip straight to large press-ups. A staged build from prone lying to elbows to press-ups is often more manageable and matches common NHS progressions shown by South Tees Hospitals NHS Foundation Trust.
Staying inactive all day
Complete bed rest is usually not the answer. Mayo Clinic notes that staying inactive can make symptoms worse, while self-care and movement often help.
Who should try McKenzie exercises for sciatica?
McKenzie exercises for sciatica may be most useful for people who:
- have pain that radiates from the low back or buttock into the leg
- notice that gentle extension reduces or centralizes symptoms
- tolerate lying on the stomach or leaning back
- want a simple home program focused on self-management
They may be less helpful for people whose symptoms clearly worsen with extension or who have a different pain pattern that responds better to another direction. A clinician trained in McKenzie can help identify your directional preference more accurately, as noted in StatPearls.
When to see a professional
See a clinician if:
- pain is severe or persistent
- symptoms are not improving after a few weeks
- you have clear weakness, numbness, or balance changes
- you are unsure whether the pain is really sciatica
Mayo Clinic advises medical evaluation for serious symptoms or symptoms lasting more than a month, and Cleveland Clinic emphasizes that sciatica can include weakness as well as pain and tingling.
Frequently asked questions
Can McKenzie exercises cure sciatica?
No single exercise method can guarantee a cure. McKenzie exercises may help manage symptoms and improve function in some people, especially when the chosen movement centralizes symptoms.
Which McKenzie exercise is best for sciatica?
For many people, the best starting point is prone lying or prone on elbows. The best overall exercise is the one that reduces leg symptoms or moves them closer to the spine.
How many times a day should I do McKenzie exercises for sciatica?
A common home pattern is 3 to 4 short sessions per day, using 5 to 10 reps or short holds depending on the exercise. University Hospitals of North Midlands commonly uses that range in patient advice.
Should McKenzie exercises make my back hurt more?
A small amount of local low-back pressure can happen, but worsening leg pain, spreading numbness, or a clear increase in symptoms is a sign to stop and reassess.
Are McKenzie press-ups good for a herniated disc?
They may help when disc-related symptoms respond well to extension. Sciatica is often linked to herniated discs, but not every herniated disc responds the same way, according to Mayo Clinic.
Is walking better than McKenzie exercises for sciatica?
Walking and McKenzie exercises can work well together. McKenzie drills help identify a symptom-relieving direction, while walking supports general activity and avoids prolonged inactivity, as noted by Mayo Clinic.
Can I do McKenzie exercises every day?
Yes, these exercises are usually done daily when they are helping and not aggravating symptoms. The key is monitoring symptom response, not pushing through worsening pain.
Conclusion
McKenzie exercises for sciatica can be a practical home strategy when your symptoms respond well to extension and become more centralized over time. Start with the gentlest option, progress slowly, and judge success by how your leg symptoms behave, not just how much effort the exercise feels like.
If you are building a sciatica routine, begin with prone lying, test the response, and only move forward when the next step clearly feels better or at least no worse.
This content is for informational purposes only and not medical advice.
