McKenzie exercises can help improve back mobility and comfort for some people, especially when the right movement direction reduces or centralizes symptoms rather than making them spread farther. That matters because the McKenzie Method is not just a random set of back exercises. It is a classification-based system, also called Mechanical Diagnosis and Therapy, that matches movement to symptom response and emphasizes self-management. The McKenzie Institute describes it as an assessment and treatment approach built around helping patients manage symptoms and recover function.

A good McKenzie routine usually starts with simple repeated movements, checks how your symptoms respond, and avoids forcing motions that clearly worsen your pattern. Recent evidence in PubMed suggests McKenzie-based care delivered by credentialed therapists may improve pain and disability in some people with low back pain, but a 2023 review in the Cochrane Library found little to no clinically important benefit for acute and subacute non-specific low back pain overall. In plain language, these exercises may help, but they are not a universal fix.
What Are McKenzie Exercises?
McKenzie exercises are repeated spinal movements or positions used to see which direction helps symptoms improve. In practice, that often means extension, flexion, or side-glide based movements, plus posture correction and self-monitoring. One important point is that “McKenzie” does not simply mean back bends. Research indexed in PubMed has specifically warned against treating the method as generic extension exercises for everyone.

A core idea is directional preference. That means one direction of movement feels better or leaves you moving better afterward. Guidance from JOSPT supports using repeated movements and exercises that match centralization and directional preference in appropriate low back pain cases.
Do McKenzie Exercises Actually Work?
The evidence is mixed but promising in the right setting. A 2025 systematic review in PubMed found low-to-moderate certainty evidence that the McKenzie Method delivered by credentialed therapists was superior to all other interventions combined for pain up to 6 months and disability up to 12 months, with some clinically important differences against exercise in the short term and minimal intervention in the intermediate term.

At the same time, a 2023 review in the Cochrane Library concluded the McKenzie method is not an effective treatment for acute and subacute non-specific low back pain as a broad group. That is why the safest claim is this: McKenzie exercises may work well for selected people, especially when repeated movement clearly improves the symptom pattern, but they should not be oversold as the best approach for every back pain case.
Who May Benefit Most From McKenzie Exercises?
McKenzie-style exercises may fit best when you notice that one movement direction consistently helps. That may include people who:
- feel better with repeated extension, flexion, or side-glide movements
- notice pain moves out of the leg and closer to the spine
- feel less stiff after repeated movement
- can self-manage mild to moderate mechanical back symptoms
- want an active approach rather than passive treatment alone
Research on centralization and directional preference in JOSPT supports the idea that symptom behavior during movement testing can help guide treatment and prognosis.
10 Best McKenzie Exercises for Back Mobility and Comfort
These are best viewed as common McKenzie-style movements, not a one-size-fits-all prescription. The right exercise is the one that improves your response pattern, not the one that looks most advanced.
1. Prone Lying
How to do it:
- Lie face down on a firm surface.
- Rest your arms by your sides or place your hands near your head.
- Relax your lower body and let your low back settle.
- Hold for 1 to 2 minutes if comfortable.
- Breathe slowly and stop if symptoms clearly worsen.
Why it works:
Prone lying is often the first step for people who may benefit from extension-based progression. It introduces gentle lumbar extension without a strong push and can help some people test whether this position feels relieving, neutral, or aggravating.
Muscles worked:
This is more of a positioning drill than a strengthening move, but it lightly exposes the lumbar spine and hip flexors to an extension posture.
Trainer Tip:
Use this as a starting point if press-ups feel too aggressive. If leg pain eases or centralizes, that is often more meaningful than whether the position feels dramatic.
2. Prone on Elbows
How to do it:
- Lie face down.
- Prop yourself up on your elbows under your shoulders.
- Keep your hips and pelvis on the floor.
- Hold for 5 to 10 seconds.
- Repeat 5 to 10 times if tolerated.
Why it works:
This is a gentle progression from prone lying. It increases extension slightly and helps you test whether a small increase in lumbar arch changes your symptoms in a favorable way.
Muscles worked:
Spinal extensors help support the position, while the front of the trunk and hips experience mild stretch.
Trainer Tip:
Do not shrug your shoulders toward your ears. Stay relaxed through the neck and let the movement come from the spine position.
3. Prone Press-Up
How to do it:
- Start face down with hands under your shoulders.
- Press through your hands to lift your chest.
- Keep your hips and pelvis down if possible.
- Go only as far as comfortable.
- Lower slowly and repeat 8 to 10 reps.
Why it works:
The prone press-up is one of the best-known McKenzie extension exercises. It creates repeated lumbar extension and may help people whose symptoms improve with extension bias.
Muscles worked:
Triceps and shoulder stabilizers assist the push, while the lumbar area moves through extension.
Trainer Tip:
Your goal is not to force a huge range. What matters most is whether symptoms move toward the center of the back or become easier afterward.
4. Sustained Extension in Lying
How to do it:
- Get into the top of a gentle press-up.
- Hold the position for 2 to 5 seconds.
- Return down slowly.
- Repeat for 5 to 8 reps.
- Keep the movement controlled and easy.
Why it works:
Some people respond better to a brief sustained end-range position than to faster reps. This can help you test whether a held extension position is more useful for stiffness and comfort.
Muscles worked:
Shoulders, arms, and trunk stabilizers support the hold while the lumbar spine stays in extension.
Trainer Tip:
Use shorter holds at first. A small hold with a good response beats a long hold that irritates symptoms.
5. Standing Back Extension
How to do it:
- Stand with feet hip-width apart.
- Place your hands on your hips or low back.
- Gently lean backward.
- Return to standing.
- Repeat 8 to 10 times.
Why it works:
This is a practical option when you cannot get on the floor. It is often used after long periods of sitting, driving, or desk work.
Muscles worked:
Spinal extensors and glutes help control the movement. The front of the hips and trunk may feel a mild stretch.
Trainer Tip:
Think of this as a reset, not a deep bend. A comfortable range is enough.
6. Lying Flexion
How to do it:
- Lie on your back with knees bent.
- Bring both knees gently toward your chest.
- Hold for 1 to 2 seconds.
- Lower your feet back down.
- Repeat 8 to 10 reps.
Why it works:
Not everyone has an extension preference. Some people do better with flexion-based movement, especially if extension feels compressive or irritating. This drill explores that possibility.
Muscles worked:
Abdominals and hip flexors help create the movement, while the lumbar area moves into flexion.
Trainer Tip:
Choose this only if it feels relieving or loosening. If it increases leg symptoms or leaves you worse afterward, it may not be your direction.
7. Single Knee to Chest
How to do it:
- Lie on your back with knees bent.
- Pull one knee toward your chest.
- Keep the other foot on the floor.
- Hold briefly, then lower.
- Repeat 6 to 8 reps per side.
Why it works:
This is a milder flexion variation than double-knee-to-chest and may be more comfortable for people who need a lower-intensity flexion-based movement.
Muscles worked:
Hip flexors and trunk muscles assist the position, while the low back moves gently into flexion.
Trainer Tip:
Move smoothly and avoid yanking the knee in. Gentle motion gives you better feedback.
8. Seated Flexion
How to do it:
- Sit on a chair with feet flat.
- Slowly bend forward and reach toward the floor.
- Pause briefly in a comfortable range.
- Return to upright.
- Repeat 8 to 10 reps.
Why it works:
This gives you a convenient way to test flexion preference during the day. It can feel more accessible than floor-based flexion work.
Muscles worked:
Abdominals assist trunk control, while the lumbar spine and hips move into flexion.
Trainer Tip:
Exhale as you fold forward. Keep the movement slow enough to notice whether it helps or aggravates symptoms.
9. Side Glide in Standing
How to do it:
- Stand next to a wall with the painful side away from the wall unless a clinician has shown you otherwise.
- Place your shoulder against the wall for support.
- Shift your hips sideways toward the wall.
- Return to center.
- Repeat 8 to 10 times.
Why it works:
A side-glide is often used when there is a visible trunk shift or when symptoms respond better to frontal-plane correction than pure flexion or extension.
Muscles worked:
Hip abductors, trunk stabilizers, and spinal support muscles help control the shift.
Trainer Tip:
This exercise is easiest to misuse alone. Be conservative with range and stop if symptoms peripheralize.
10. Extension With Side Bias
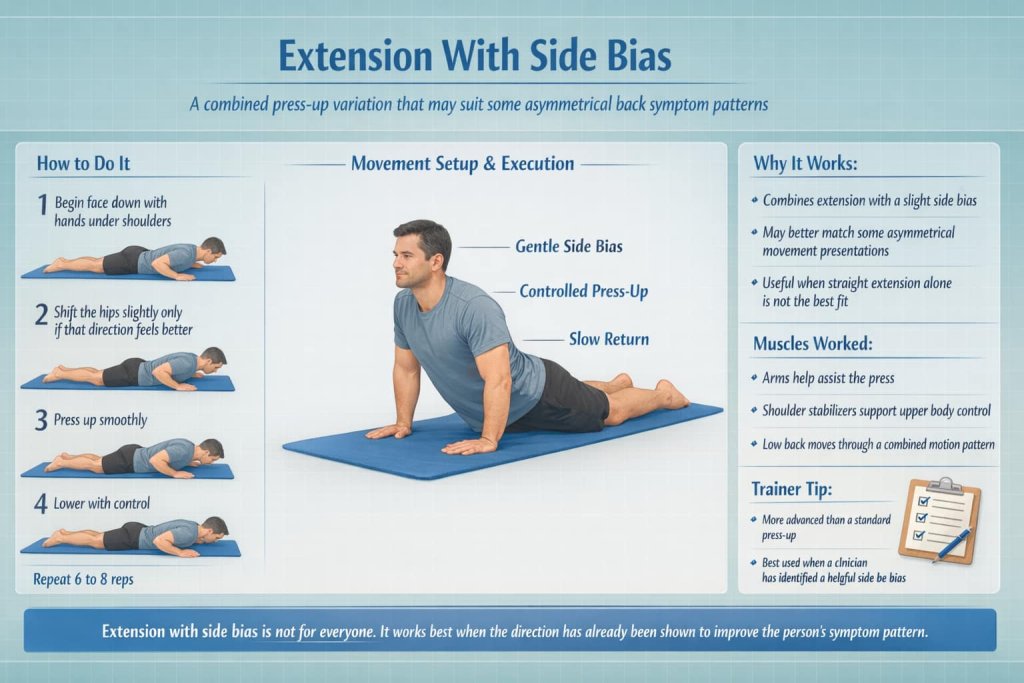
How to do it:
- Begin in a prone press-up position.
- Shift your hips slightly to one side before pressing up if that direction feels better.
- Press up gently.
- Lower under control.
- Repeat 6 to 8 reps.
Why it works:
Some people need a combined movement rather than straight extension. A side-biased press-up can better match an asymmetrical presentation.
Muscles worked:
Arms and shoulder stabilizers assist the press, while the low back moves through a combined pattern.
Trainer Tip:
This is a more advanced self-management option. It is best used when a clinician has already helped identify a helpful side bias.
Before You Start McKenzie Exercises
Start gently and pay close attention to symptom response. Many self-care back pain guidelines support staying active and using exercise as part of management, but they also emphasize that care should be individualized. Guidance from NICE recommends exercise as part of low back pain management rather than relying on passive care alone.
Use these simple rules before you begin:
- Stop if pain sharply increases and stays worse.
- Stop if symptoms spread farther down the leg.
- Get urgent medical care for new bladder or bowel changes, new saddle numbness, or worsening leg weakness.
- Use slow, controlled reps.
- Never force end range.
Emergency warning resources from the NHS highlight red-flag symptoms such as altered saddle sensation, urinary retention or incontinence, bowel changes, and new leg weakness.
How to Know Whether a McKenzie Exercise Is Helping
A McKenzie-style movement may be a good fit when:
- pain becomes more centered in the low back
- leg pain decreases or moves upward
- stiffness eases after several reps
- you can stand, walk, or sit more comfortably afterward
- the movement becomes easier over time
A poor response usually looks like:
- symptoms spreading farther down the leg
- sharper pain that stays worse after stopping
- new numbness, tingling, or weakness
- a clear loss of function after the session
This symptom pattern approach is consistent with the directional preference and centralization literature in JOSPT.
Common Mistakes to Avoid With McKenzie Exercises
Doing the most famous movement instead of the right movement
Many people assume McKenzie means repeated back extension only. That is inaccurate. The method is based on classification and symptom response, not a fixed routine for everyone. Research indexed in PubMed supports that distinction.
Forcing pain
These exercises should challenge movement, not create a dramatic flare. Pushing into a strong worsening response usually makes self-management less useful.
Ignoring red flags
Exercise is not appropriate for every situation. Seek prompt medical evaluation if you have severe trauma, fever, unexplained weight loss, cancer history, new bladder or bowel problems, saddle numbness, or worsening neurological symptoms. Guidance from the NHS and NHS spinal emergency resources supports urgent assessment for these warning signs.
Doing too many reps too soon
Repeated movement can be useful, but more is not always better. Start with a small number of controlled reps and reassess.
A Simple McKenzie Exercise Routine for Beginners
Try this gentle sequence once or twice a day if it suits your symptom pattern:
- Prone lying for 1 to 2 minutes
- Prone on elbows for 5 reps
- Prone press-ups for 8 reps
- Standing back extensions for 8 reps during the day after sitting
If flexion clearly feels better than extension, you could instead try:
- Single knee to chest for 6 reps each side
- Lying flexion for 8 reps
- Seated flexion for 8 reps
The key is not to do both directions aggressively at the same time. Choose the direction that leaves you moving and feeling better afterward.
When to See a Physical Therapist Instead of Self-Treating
See a clinician if:
- your pain has not improved after 1 to 2 weeks of careful self-management
- you are not sure which direction helps
- leg symptoms are significant
- you keep having recurrent flare-ups
- you have numbness, weakness, or walking difficulty
- you want a proper MDT assessment
The strongest 2025 evidence in PubMed was specifically for the McKenzie Method delivered by credentialed therapists, which is a useful reminder that expert assessment can matter.
FAQ About McKenzie Exercises
Are McKenzie exercises only for low back pain?
No. The McKenzie Method is used for spinal and even some extremity problems, but this article focuses on low back mobility and comfort. The method itself is broader than one body region, as explained by the McKenzie Institute.
Are McKenzie exercises the same as extension exercises?
No. Extension is common, but McKenzie care can also include flexion, side-glide, posture correction, and other direction-specific movements based on assessment. Research indexed in PubMed makes that clear.
How often should I do McKenzie exercises?
That depends on the movement and your response. In self-care settings, people often use a small number of controlled reps several times a day, but the best frequency is the one that improves symptoms without causing a lasting flare.
Can McKenzie exercises make back pain worse?
Yes, the wrong movement direction can worsen symptoms. That is why it is important to monitor whether pain centralizes or spreads. Stop if the pattern is clearly worse afterward.
Which McKenzie exercise is best?
There is no universal best exercise. The best one is the movement that improves your symptoms, mobility, or comfort without causing peripheralization.
Should I do McKenzie exercises if pain goes down my leg?
Sometimes, but with caution. Referred pain or sciatica symptoms can respond to repeated movement in some cases, yet worsening leg pain, increasing numbness, or weakness should push you toward professional evaluation.
How long does it take for McKenzie exercises to help?
Some people notice a response within one session or a few days. Others may not respond at all because their directional preference is different or the problem needs another approach.
Conclusion
McKenzie exercises can be a helpful tool for improving back mobility and comfort, but the right movement matters more than the name of the exercise. Start with simple, controlled reps, pay attention to whether symptoms centralize or worsen, and do not assume extension is automatically best. If your response is unclear or symptoms are more severe, a credentialed clinician can help identify the most useful direction and build a safer plan.
