McKenzie back exercises may help relieve lower back pain by using repeated movements to find the direction that reduces or “centralizes” your symptoms. This matters because the McKenzie Method (also called Mechanical Diagnosis and Therapy, MDT) is designed to match movements to how your pain behaves, not just to “stretch everything.”
For the safest results, you’ll use simple symptom rules (better, worse, or unchanged) and stop if pain spreads or sharpens.

If you want the official overview of MDT, you can review it through the McKenzie Institute International, which explains how the system identifies directional preference and centralization.
What Are McKenzie Back Exercises
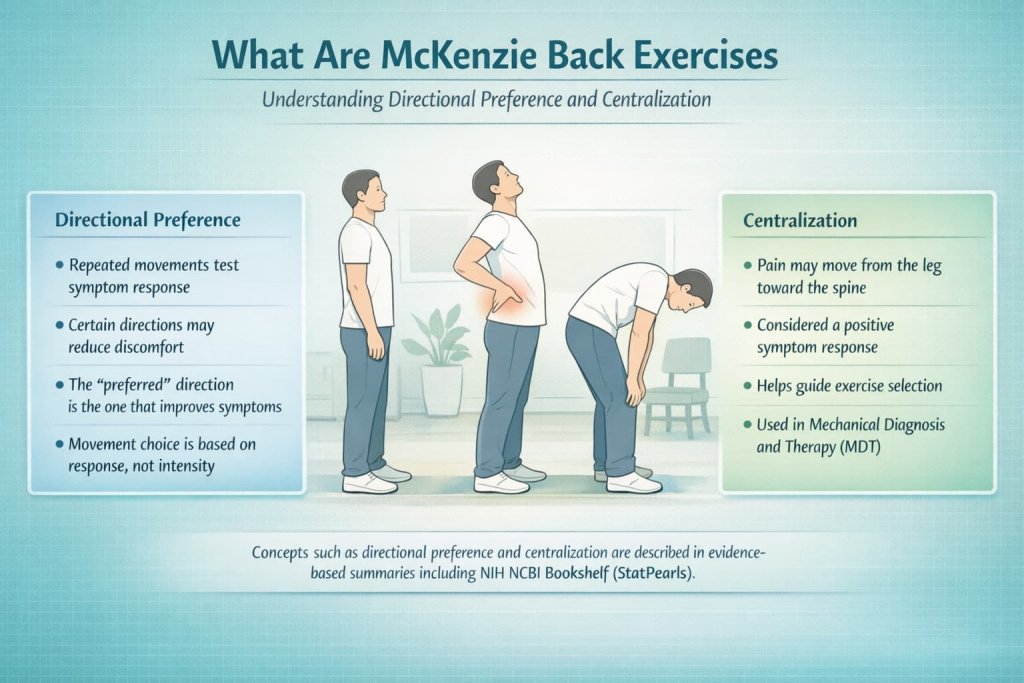
McKenzie back exercises are repeated movements (and posture adjustments) commonly used in MDT to help identify a “directional preference”—the movement direction that reduces symptoms. A key concept is “centralization,” where pain that travels into the buttock or leg moves closer to the spine with certain movements, a concept summarized in the NIH NCBI Bookshelf (StatPearls).
Who These Exercises May Help Most
McKenzie-style exercises may be a fit if you notice:

- Your pain changes clearly with posture (sitting vs. standing) or repeated movement
- Your leg pain improves (moves closer to your back) with certain positions
- You prefer a structured “test-and-respond” routine rather than random stretching
Physical therapy clinical practice guidelines discuss repeated movements and directional preference approaches as one option within nonpharmacologic care for low back pain, as outlined by the Journal of Orthopaedic & Sports Physical Therapy (JOSPT).
8 McKenzie Back Exercises
Important: These are commonly used McKenzie-style movements. The “best” one is the one that improves your symptoms (often by centralizing them). If an exercise consistently worsens pain or pushes symptoms farther down the leg, stop and seek professional guidance.
1) Prone Lying
How to do it:
- Lie on your stomach on a firm bed or mat
- Keep your legs relaxed with feet slightly turned outward
- Rest your head on your hands or a small towel
- Stay in this position for 1–3 minutes while breathing slowly
Why it works:
This is a gentle starting position that may help calm symptoms and introduce your spine to extension in a low-load way. It allows the lower back to settle without active muscular effort, which can be helpful at the beginning of a flare-up if extension feels relieving.
Muscles worked:
Low-level activation of spinal stabilizers with minimal loading. Most muscles remain relaxed in this position.
Trainer Tip:
If lying flat feels uncomfortable, place a thin pillow under your hips for the first few sessions and gradually reduce support as tolerated.
2) Prone on Elbows
How to do it:
- From prone lying, prop yourself up onto your elbows
- Keep your hips in contact with the surface
- Let your lower back relax into gentle extension
- Hold 10–30 seconds and repeat 5–10 times
Why it works:
This position introduces mild lumbar extension without forcing the movement. It serves as a progression from prone lying and can help you determine whether extension reduces or centralizes your symptoms.
Muscles worked:
Light activation of spinal extensors, along with shoulder and upper back muscles supporting the position.
Trainer Tip:
Focus on relaxing into the stretch rather than pushing aggressively upward. Breathing should remain steady and controlled.
3) Prone Press-Up
How to do it:
- Lie on your stomach with hands under your shoulders
- Press your upper body upward while keeping hips on the floor
- Pause 1–2 seconds at the top
- Lower back down with control
- Perform 8–12 repetitions
Why it works:
Repeated extension may help reduce symptoms for individuals whose pain improves with backward bending movements. It allows you to test whether extension centralizes discomfort toward the spine.
Muscles worked:
Triceps and shoulders provide support, while spinal extensors position the back. Core stabilizers assist lightly.
Trainer Tip:
Keep your glutes relaxed and avoid lifting your hips off the surface. The movement should feel controlled, not forced.
4) Standing Back Extension
How to do it:
- Stand tall with feet hip-width apart
- Place your hands on your lower back for support
- Gently lean backward within a comfortable range
- Return to neutral
- Repeat 10 times
Why it works:
This simple extension drill can serve as a posture reset after prolonged sitting. It reintroduces spinal extension in a functional, upright position.
Muscles worked:
Light engagement of spinal extensors and glutes, along with postural support muscles.
Trainer Tip:
Use a small, comfortable range of motion. If you feel compression or sharp discomfort, reduce the depth of the movement.
5) Lying Flexion (Knees-to-Chest)
How to do it:
- Lie on your back with knees bent
- Bring one knee toward your chest
- Hold briefly, then switch sides
- Repeat 5–8 times
Why it works:
Some individuals respond better to flexion-based movements. If bending forward reduces stiffness or discomfort, this gentle flexion drill may feel supportive.
Muscles worked:
Light activation of hip flexors and abdominal stabilizers, with a stretch effect on the lower back and glutes.
Trainer Tip:
Pay attention to how you feel when standing afterward. If pain increases or spreads, flexion may not be your best directional preference.
6) Seated Flexion
How to do it:
- Sit upright with feet flat on the floor
- Slowly bend forward, sliding your hands down your thighs
- Return to upright
- Perform 10 repetitions
Why it works:
This is a convenient flexion drill that may help if extension aggravates your symptoms. It provides controlled spinal flexion in a seated position.
Muscles worked:
Lower back and hip muscles in a lengthened position, with light abdominal engagement.
Trainer Tip:
Keep the movement slow and controlled. Let your symptom response guide the range of motion.
7) Side Glide in Standing
How to do it:
- Stand next to a wall
- Keep your shoulders level
- Gently shift your hips sideways toward the wall
- Return to center
- Repeat 10–15 times
Why it works:
Lateral movement may be helpful if your symptoms improve with side-bending or if you have a visible side shift. It introduces controlled frontal-plane motion.
Muscles worked:
Obliques and lateral trunk stabilizers with light engagement of hip stabilizers.
Trainer Tip:
This movement is highly individual. If you are unsure about proper alignment or symptom response, consult a qualified professional.
8) Sustained Extension Hold
How to do it:
- Choose prone on elbows or the top position of a press-up
- Hold the position for 20–60 seconds
- Rest briefly
- Repeat 3–5 times
Why it works:
Holding an extension position may provide longer exposure to the movement direction that reduces symptoms. Sustained positioning can sometimes reinforce symptom relief.
Muscles worked:
Postural endurance muscles with minimal dynamic effort.
Trainer Tip:
If symptoms increase during the hold, shorten the duration or return to a gentler variation.
How to Choose the Right McKenzie Exercise for Your Symptoms
The right McKenzie exercise is the one that improves your symptoms — not the one that feels the strongest stretch. Pay attention to how your pain responds to repeated movement.
- If extension (backward bending) reduces pain or moves it closer to your spine, focus on prone lying, prone on elbows, or press-ups.
- If flexion (forward bending) feels better, use knees-to-chest or seated flexion.
- If pain centralizes (moves toward the spine), continue.
- If pain spreads down the leg or worsens, stop.
When in doubt, consult a qualified healthcare professional for guidance.
A Simple McKenzie-Style Routine
If extension reduces symptoms:
- Prone lying: 1–2 minutes
- Prone on elbows: 5–10 holds
- Press-ups: 8–12 reps
- Standing back extension: 10 reps
If flexion reduces symptoms:
- Knees-to-chest: 5–8 reps
- Seated flexion: 10 reps
- Reassess how you feel when standing or walking
Common Mistakes to Avoid
- Choosing exercises without checking symptom response
- Forcing large ranges of motion
- Ignoring pain that spreads down the leg
- Overtraining during flare-ups
- Skipping posture corrections
Important Safety Guidelines Before Trying McKenzie Back Exercises
Use these safety rules every time:
- Work in a pain range you can control and breathe through (no forcing)
- Stop if symptoms spread farther down the leg, or numbness/weakness increases
- Move slowly for the first 2–3 reps, then repeat only if symptoms improve or centralize
- If you have a known spine condition, recent injury, or severe pain, get clinician guidance first
Research results vary by person and condition. A systematic review published by Cochrane found that for (sub)acute non-specific low back pain, the McKenzie Method may provide little to no clinically important benefit compared with other approaches in the short term, reinforcing the need to individualize and monitor symptoms carefully.
When to See a Doctor for Lower Back Pain
Seek urgent medical care if you have back pain with symptoms such as numbness or tingling around your genitals or buttocks, new bladder or bowel control problems, or severe weakness—warning signs highlighted by the NHS.
You should also contact a medical professional if your pain follows a major fall or injury, you develop fever, or you experience worsening numbness or weakness, as explained by MedlinePlus.
FAQs About McKenzie Back Exercises
Are McKenzie back exercises safe for everyone?
No. They are not appropriate for certain red-flag symptoms or severe neurological issues. Seek medical advice if unsure.
How often should I perform these exercises?
Short sessions once to three times daily are common, depending on symptom response.
What does centralization mean?
It refers to pain moving from the leg or buttock back toward the spine during movement.
Should I do press-ups if I have leg pain?
Only if symptoms improve or centralize. Stop if pain travels farther down the leg.
Can I combine these exercises with strengthening?
Often yes, but it is best to first identify movements that reduce symptoms.
How long should I try this approach?
If symptoms are not improving within a reasonable period or are worsening, seek professional evaluation.
Conclusion
McKenzie back exercises offer a structured way to test which spinal movements may help reduce lower back pain. The key is to follow symptom response carefully and avoid forcing movements. If pain persists, worsens, or includes neurological symptoms, consult a qualified healthcare professional.
This content is for informational purposes only and not medical advice.
