Meralgia paresthetica exercises are gentle, targeted movements designed to reduce nerve irritation and improve comfort in the outer thigh. When chosen carefully, these exercises may help reduce tingling, burning, or numbness by easing tension around the hip and supporting better pelvic control.
Understanding which exercises are appropriate matters because meralgia paresthetica is caused by compression of a sensory nerve—not muscle damage. The goal is to reduce pressure, improve movement tolerance, and support daily function without aggravating symptoms.
Below is a structured, evidence-informed guide to the 6 best meralgia paresthetica exercises, along with safety guidance and FAQs.
What Is Meralgia Paresthetica?
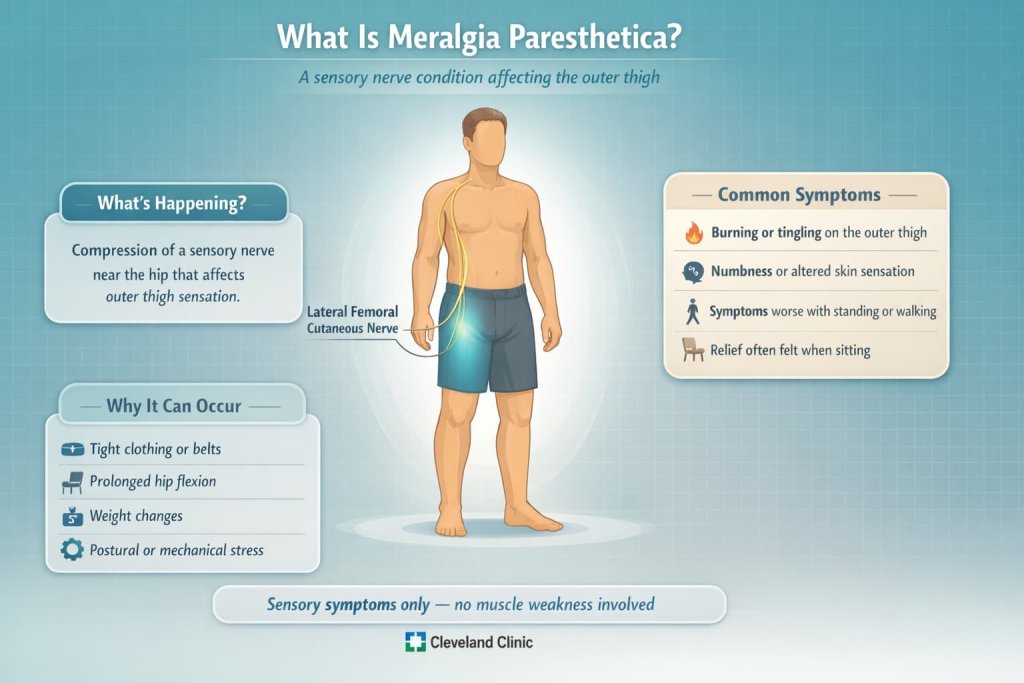
Meralgia paresthetica occurs when the lateral femoral cutaneous nerve becomes compressed as it passes near the front of the hip and pelvis. This nerve provides sensation to the outer thigh, so symptoms are sensory rather than muscular.
Common features include:
- Burning or tingling on the outer thigh
- Numbness or altered skin sensation
- Symptoms that worsen with standing or walking and ease with sitting
Medical sources such as the Cleveland Clinic note that tight clothing, prolonged hip flexion, weight changes, or postural stress may contribute to nerve compression.
How Exercise May Help Meralgia Paresthetica

Exercise does not “fix” the nerve itself, but it may help by:
- Reducing tension in tissues around the front and side of the hip
- Supporting hip and pelvic stability during standing and walking
- Improving movement confidence and daily activity tolerance
Physical therapy guidance published through ChoosePT highlights that carefully selected mobility and strengthening exercises are often used as part of conservative management when symptoms allow.
6 Best Meralgia Paresthetica Exercises
These six exercises focus on reducing hip tension, improving pelvic stability, and supporting nerve comfort around the outer thigh. All movements are gentle, symptom-guided, and designed to be performed safely as part of conservative care.
1. Standing Hip Flexor Stretch
How to do it
- Stand in a split stance with the affected leg positioned behind you
- Keep your chest tall and pelvis facing forward
- Gently bend the front knee without leaning forward
- Lightly squeeze the glute on the back leg to avoid arching the lower back
- Hold a comfortable stretch at the front of the hip for 20–30 seconds
- Repeat 2–3 times, staying within a pain-free range
Why it works
Tight hip flexors can increase tension near the front of the pelvis where the lateral femoral cutaneous nerve passes. This sustained tension may worsen nerve irritation during standing or walking. Gentle hip flexor stretching may help reduce pressure in this region and improve tolerance to upright activities.
Trainer Tip
Focus on posture rather than depth. A mild stretch sensation is sufficient—sharp, burning, or radiating symptoms indicate excessive tension and should be avoided.
2. Tensor Fasciae Latae (TFL) Stretch
How to do it
- Stand upright with feet hip-width apart
- Cross the affected leg slightly behind the other leg
- Gently shift your hips away from the affected side
- Keep your torso upright and shoulders relaxed
- Hold the stretch along the outer front hip for 20–30 seconds
- Breathe slowly and repeat as tolerated
Why it works
The tensor fasciae latae lies close to the nerve’s pathway as it travels toward the outer thigh. Excess tension in this muscle may contribute to local compression. Stretching the TFL may help reduce lateral hip tightness and improve comfort during standing and walking.
Trainer Tip
This stretch should feel broad and diffused across the hip—not sharp or localized. If symptoms intensify, reduce the range or discontinue.
3. Side-Lying Hip Abduction
How to do it
- Lie on your side with the affected leg on top
- Keep your hips stacked and spine neutral
- Straighten the top leg and slightly angle it backward
- Lift the leg slowly to a comfortable height
- Lower with control and repeat for 8–12 repetitions
Why it works
Weak lateral hip muscles can lead to poor pelvic control during walking, which may increase strain near the hip crease. Strengthening the hip abductors supports pelvic stability and may reduce repetitive stress around the nerve’s pathway.
Trainer Tip
Quality matters more than height. Small, slow lifts with good control are more effective than high or fast movements.
4. Glute Bridge
How to do it
- Lie on your back with knees bent and feet flat on the floor
- Place your feet about hip-width apart
- Gently brace your core and squeeze your glutes
- Lift your hips until your torso and thighs form a straight line
- Pause briefly, then lower slowly with control
- Perform 8–12 repetitions
Why it works
Stronger glute muscles reduce overreliance on the hip flexors during standing, walking, and posture maintenance. This balanced muscle activation may help reduce mechanical stress around the front of the pelvis.
Trainer Tip
Avoid pushing through your lower back. If you feel the movement primarily in your spine instead of your glutes, reduce the height.
5. Pelvic Tilt Exercise
How to do it
- Lie on your back with knees bent and feet on the floor
- Gently tighten your abdominal muscles
- Flatten your lower back into the floor by tilting the pelvis
- Hold for 3–5 seconds
- Relax fully and repeat for 8–10 repetitions
Why it works
Pelvic tilts promote awareness and control of pelvic position. Improved control may help reduce prolonged hip flexion and excessive anterior pelvic tilt, both of which can increase nerve sensitivity in some individuals.
Trainer Tip
This is a subtle movement. Focus on control and breathing rather than force or intensity.
6. Gentle Nerve Glide (Only If Tolerated)
How to do it
- Lie comfortably on your back
- Slowly straighten the affected leg while keeping the pelvis relaxed
- Gently bend and straighten the knee within a comfortable range
- Move slowly and stop immediately if symptoms increase
- Perform only a few controlled repetitions
Why it works
In some cases, gentle nerve-friendly movement may support normal mobility of the nerve within surrounding tissues. This approach is sometimes used in physical therapy when symptoms are stable and well-tolerated.
Trainer Tip
Nerve glides should never provoke symptoms. If burning, tingling, or numbness increases, stop and consult a qualified professional before continuing.
How Often Should You Do Meralgia Paresthetica Exercises?
Most meralgia paresthetica exercise programs focus on consistency rather than intensity. Because the condition involves nerve sensitivity rather than muscle weakness alone, exercises should be performed in a way that supports comfort and avoids irritation.
General frequency guidance:
- Gentle mobility and stretching exercises may be done daily if they remain symptom-free
- Strengthening exercises are typically performed 2–4 times per week, allowing rest days between sessions
- Each exercise should be completed for low to moderate repetitions, staying well within a comfortable range
Symptoms should always guide frequency. If tingling, burning, or numbness increases during or after exercise, reduce volume or take a break.
What to Avoid With Meralgia Paresthetica
Certain activities and habits may increase pressure on the lateral femoral cutaneous nerve and worsen symptoms. Avoiding these factors is often just as important as choosing the right exercises.
Common things to avoid include:
- Tight belts, waistbands, shapewear, or compressive clothing
- Prolonged hip flexion, such as long periods of sitting without breaks
- Exercises that require heavy loading across the hips or waist
- Aggressive stretching that produces sharp, burning, or radiating sensations
- Sudden increases in exercise intensity or volume
Movements that significantly increase symptoms should be modified or paused. Conservative care guidance from sources like the Cleveland Clinic notes that reducing mechanical compression is a key part of symptom management.
When to Seek Medical or Physical Therapy Guidance
While many people improve with conservative care, professional evaluation is important in certain situations. Seeking medical or physical therapy guidance helps confirm the diagnosis and ensures that symptoms are not caused by another condition.
You should consult a healthcare professional if:
- Symptoms persist or worsen despite activity modification and gentle exercise
- Numbness becomes constant or spreads beyond the outer thigh
- Pain interferes with walking, sleep, or daily activities
- Symptoms develop suddenly without a clear trigger
A qualified clinician or physical therapist can assess posture, movement patterns, and contributing factors, and design an individualized plan. Medical organizations such as the American Academy of Orthopaedic Surgeons and American Physical Therapy Association recommend professional guidance when symptoms do not improve with initial conservative strategies.
Safety Guidelines Before Starting
Before beginning meralgia paresthetica exercises:
- Avoid tight waistbands, belts, or compressive clothing
- Stay within a symptom-free or symptom-light range
- Stop any exercise that increases burning, tingling, or numbness
Organizations such as the American Academy of Orthopaedic Surgeons emphasize that persistent or worsening symptoms should be medically evaluated.
Frequently Asked Questions
Can exercise cure meralgia paresthetica?
Exercise does not cure the condition, but it may help reduce contributing factors and support symptom management.
How often should I do these exercises?
Most programs use light daily mobility and strengthening 3–5 days per week, based on tolerance.
Should I stretch if I feel numbness?
Stretching should remain gentle. Increased numbness or burning is a sign to stop.
Is walking good or bad for meralgia paresthetica?
Walking is often tolerated, especially with posture awareness and breaks, but symptoms should guide duration.
Can weight training make it worse?
Heavy lifting that increases waist or hip compression may aggravate symptoms in some people.
Do I need physical therapy?
Many people benefit from guided physical therapy, especially if symptoms persist.
Conclusion
Meralgia paresthetica exercises focus on reducing hip tension, improving pelvic stability, and supporting nerve comfort—not forcing aggressive movement. When done gently and consistently, these exercises may help improve daily comfort and mobility.
If symptoms continue or worsen, seek professional guidance to ensure the safest and most effective approach.
This content is for informational purposes only and not medical advice.
