Piriformis syndrome exercises may help reduce buttock pain, hip tightness, and sciatica-like symptoms when they focus on gentle stretching, mobility, and hip stability. That matters because piriformis-related pain can feel similar to other causes of sciatica, so the goal is not to force the area, but to move in ways that may ease irritation and improve daily function. Guidance from the NHS and recent review literature supports gentle exercise as part of conservative care.

If symptoms are truly coming from the piriformis area, the most useful routine usually includes a few key pieces: gentle stretches, light hip mobility, glute strengthening, and less prolonged sitting. This article walks through 10 practical exercises, how to do them safely, and when you should stop and get medical advice.
What are piriformis syndrome exercises?
Piriformis syndrome exercises are movements used to gently stretch the piriformis muscle and improve strength and control in the hips and core. The piriformis sits deep in the buttock and lies close to the sciatic nerve. When that area becomes irritated, symptoms may include buttock pain, tightness, and pain, tingling, or numbness traveling down the leg. According to Cleveland Clinic, home exercise and physical therapy often focus on stretching and strengthening.
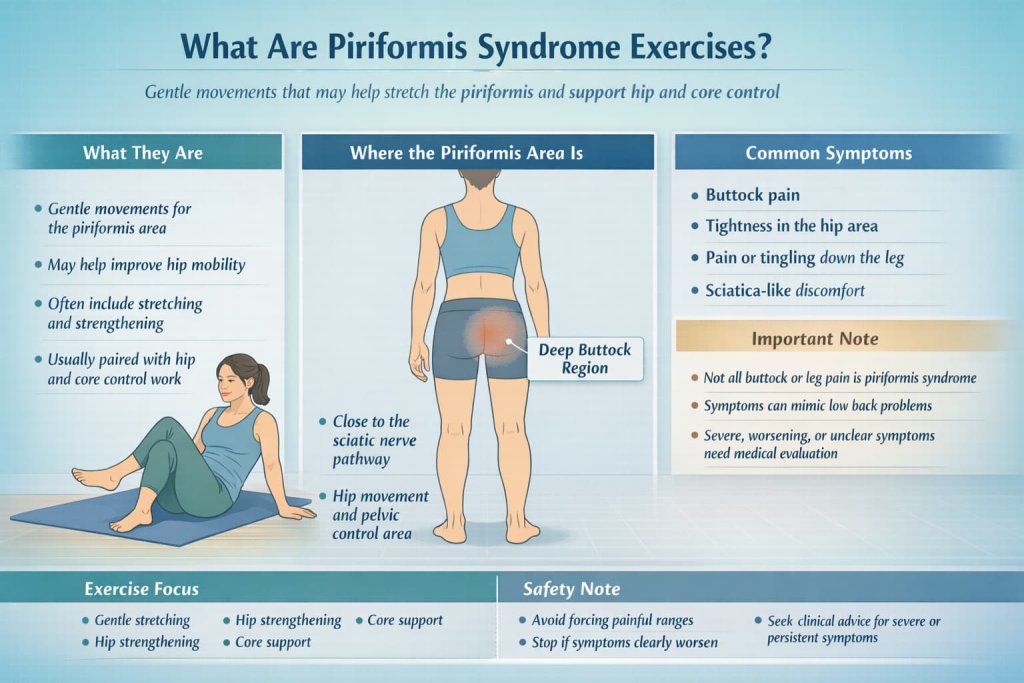
A practical point is important here: not every case of buttock pain or leg pain is piriformis syndrome. The condition can mimic low back problems and other causes of sciatica, which is one reason symptoms that are severe, worsening, or unclear should be evaluated by a clinician.
Do piriformis syndrome exercises actually help?
They may help, especially as part of conservative care, but they are not a guaranteed fix for every cause of sciatica-like pain. A 2024 review in PMC describes stretching and hip-stabilizing physical therapy as a core part of treatment, though the overall research base is still limited.
Key takeaway:

- Severe or persistent symptoms need medical assessment
- May help reduce tightness and improve function
- Work best as part of a broader rehab approach
- Are not the right answer for every type of sciatica-like pain
Before you start piriformis syndrome exercises
The NHS says these kinds of exercises are general exercises only, are suitable for most people in good health with a reasonable level of fitness, and should be stopped immediately if they cause pain or make you feel unwell.
Start with these rules:
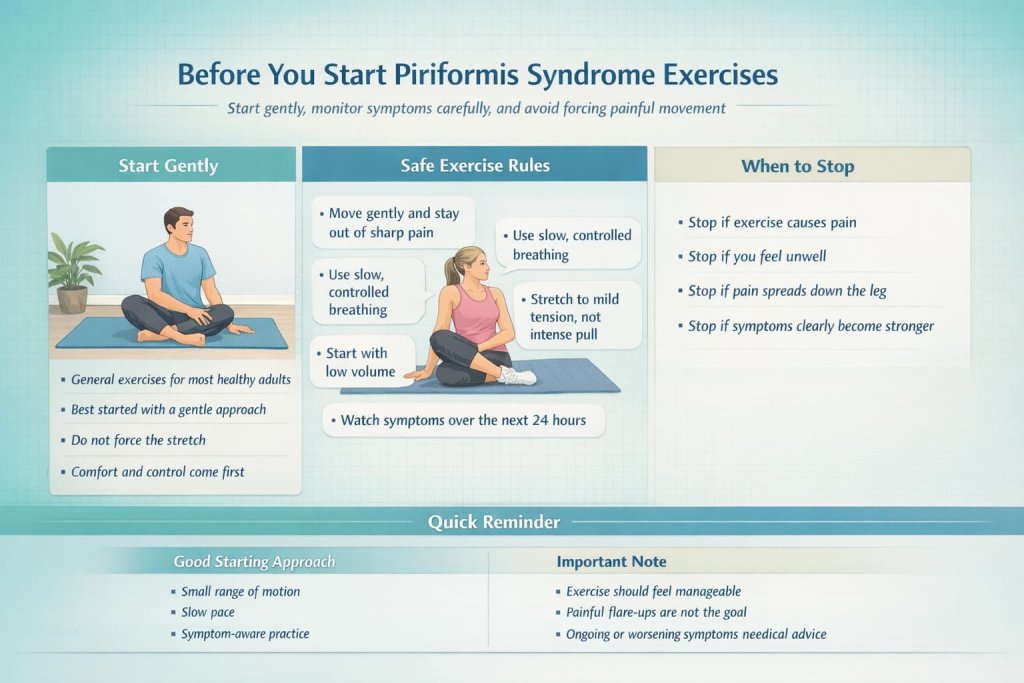
- Move gently and stay out of sharp pain
- Use slow, controlled breathing
- Stretch to mild tension, not an intense pull
- Begin with low volume and see how symptoms respond over the next 24 hours
- Stop if pain clearly spreads farther down the leg or symptoms become stronger
10 best piriformis syndrome exercises
These 10 piriformis syndrome exercises may help reduce tightness, improve hip mobility, and ease sciatica-like discomfort. The list includes a mix of gentle stretches and strengthening moves to support better movement and daily comfort.
1. Knee-to-opposite-shoulder piriformis stretch
How to do it:
- Lie on your back with both legs straight.
- Bend the affected leg.
- Use the opposite hand to gently pull that knee toward the opposite shoulder.
- Hold for 20 to 30 seconds.
- Repeat 2 to 4 times per side.
Why it works:
This is one of the most commonly recommended piriformis stretches because it targets the deep buttock area directly. Cleveland Clinic includes this among its top physical therapy-style stretches for piriformis syndrome.
Muscles worked:
Piriformis, deep hip rotators, gluteal region.
Trainer Tip:
Keep your low back relaxed on the floor. Do not yank the knee across your body.
2. Supine figure-4 stretch
How to do it:
- Lie on your back with both knees bent.
- Cross the ankle of the affected side over the opposite knee.
- Reach through and hold the back of the supporting thigh.
- Gently pull the leg toward your chest.
- Hold for 20 to 30 seconds.
- Repeat 2 to 4 times.
Why it works:
This stretch opens the outer hip and is often easier to control than more aggressive twisting stretches. It is also one of the best-known piriformis options in clinical exercise guides.
Muscles worked:
Piriformis, gluteus maximus, gluteus medius, deep hip rotators.
Trainer Tip:
Keep the stretch smooth and moderate. If you feel pinching in the front of the hip, reduce the range.
3. Seated figure-4 stretch
How to do it:
- Sit tall on a chair.
- Place the ankle of the affected side over the opposite knee.
- Keep your spine long and gently lean forward from the hips.
- Stop when you feel a mild stretch in the buttock.
- Hold for 20 to 30 seconds.
- Repeat 2 to 4 times.
Why it works:
This is a convenient option for people who sit a lot and need a simple movement break during the day. Since prolonged sitting can aggravate piriformis symptoms, a seated stretch may be useful between work periods.
Muscles worked:
Piriformis, glutes, posterior hip tissues.
Trainer Tip:
Do not round your whole back just to go lower. Lean from the hips.
4. Supine hip rotation windshield wipers
How to do it:
- Lie on your back with knees bent and feet flat.
- Keep the movement small at first.
- Let both knees slowly move side to side.
- Stay in a comfortable range.
- Perform 8 to 12 slow reps.
Why it works:
Gentle hip rotation can help reduce stiffness around the deep glute area without the intensity of a long hold stretch. It is a useful early option when the area feels tight but reactive.
Muscles worked:
Hip rotators, glutes, pelvic stabilizers.
Trainer Tip:
This should feel like light mobility work, not a forced stretch.
5. Bridge
How to do it:
- Lie on your back with knees bent and feet hip-width apart.
- Tighten your abdominal wall lightly.
- Press through your feet and lift your hips.
- Pause briefly at the top.
- Lower with control.
- Perform 8 to 12 reps.
Why it works:
A bridge helps strengthen the glutes and posterior chain. That matters because rehab for piriformis-related pain is not only about stretching. Strengthening the muscles around the hips can improve control and reduce overload on irritated tissues. Recent review literature specifically highlights strengthening the piriformis and other hip stabilizers.
Muscles worked:
Gluteus maximus, hamstrings, core, posterior hip stabilizers.
Trainer Tip:
Lift only as high as you can without cramping or low-back arching.
6. Clamshell
How to do it:
- Lie on your side with knees bent and feet together.
- Keep your hips stacked.
- Lift the top knee without letting your pelvis roll backward.
- Lower slowly.
- Perform 10 to 15 reps per side.
Why it works:
Clamshells train the lateral hip muscles that help stabilize the pelvis. Better hip control may reduce stress in the deep glute region during walking, standing, and stairs.
Muscles worked:
Gluteus medius, gluteus minimus, deep hip external rotators.
Trainer Tip:
Think about moving from the hip, not from the low back.
7. Side-lying hip abduction
How to do it:
- Lie on your side with the bottom leg bent for support and the top leg straight.
- Keep the top foot facing forward.
- Lift the top leg slowly.
- Pause, then lower with control.
- Perform 8 to 12 reps per side.
Why it works:
This movement builds strength in the hip abductors, especially the gluteus medius. That can support pelvis control and reduce compensations that may aggravate buttock pain.
Muscles worked:
Gluteus medius, gluteus minimus, tensor fasciae latae.
Trainer Tip:
Do not let the toes turn upward too much. Keep the leg slightly behind your torso.
8. Bird dog
How to do it:
- Start on hands and knees.
- Brace your midsection gently.
- Reach one arm forward and the opposite leg back.
- Hold for a brief pause.
- Return and switch sides.
- Perform 6 to 10 reps per side.
Why it works:
Cleveland Clinic recommends including core work because a stronger core can support the piriformis region. Bird dog is a controlled, low-load way to build trunk and hip stability.
Muscles worked:
Core, glutes, spinal stabilizers, shoulder stabilizers.
Trainer Tip:
Keep your hips level. The goal is control, not height.
9. Standing small-range squat
How to do it:
- Stand with feet about shoulder-width apart.
- Push your hips back slightly.
- Bend the knees into a small, comfortable squat.
- Stand back up with control.
- Perform 8 to 10 reps.
Why it works:
Cleveland Clinic includes a small-range squat as a practical strengthening move. It trains the hips and legs without requiring deep positions that may irritate symptoms.
Muscles worked:
Glutes, quadriceps, hamstrings, core.
Trainer Tip:
Keep the range small at first. Pain-free quality matters more than depth.
10. Walking
How to do it:
- Start with a short, easy walk.
- Use a pace that does not increase symptoms.
- Aim for even steps and relaxed posture.
- Stop and rest if symptoms rise.
- Gradually build duration over time.
Why it works:
Cleveland Clinic notes that walking is one of the better cardio choices for piriformis syndrome. Gentle walking may help reduce stiffness from prolonged sitting and keeps you moving without prolonged compression in one position.
Muscles worked:
Glutes, calves, core, hip stabilizers.
Trainer Tip:
A shorter walk done consistently is often better than a long walk that flares symptoms.
A simple piriformis syndrome exercise routine
You do not need to do all 10 exercises every day. A simple starting plan may look like this:
Option 1: Flare-up-friendly routine
- Knee-to-opposite-shoulder stretch
- Supine figure-4 stretch
- Hip rotation windshield wipers
- Easy walking
Option 2: Mobility plus strength routine
- Seated figure-4 stretch
- Bridge
- Clamshell
- Bird dog
- Walking
Option 3: Return-to-activity routine
- Supine figure-4 stretch
- Bridge
- Side-lying hip abduction
- Small-range squat
- Walking
Start with 1 set of each movement and see how your body responds before adding more.
How often should you do piriformis syndrome exercises?
A gentle routine is usually more helpful than an aggressive one. Cleveland Clinic’s examples often use stretching holds of about 30 seconds and strengthening work once or twice daily, while the NHS emphasizes that exercises should stop if they cause pain.
A practical approach is:
- Stretching: 1 to 2 times per day
- Strengthening: 3 to 5 days per week
- Walking or light movement: most days, as tolerated
What to avoid when symptoms are irritated
Long periods of sitting can increase pressure on the piriformis region, and Cleveland Clinic specifically advises avoiding prolonged sitting and being cautious with activities like biking if they aggravate symptoms.
You may need to temporarily reduce:
- prolonged sitting without breaks
- deep painful squats
- high-intensity hill running
- cycling if seated pressure clearly makes symptoms worse
- stretching so hard that symptoms travel farther down the leg
When to stop piriformis syndrome exercises and get medical help
Get medical advice promptly if you have severe or worsening pain, growing numbness, progressive leg weakness, or you are not sure the problem is actually piriformis syndrome. The AAOS notes that sciatica can include weakness, numbness, and burning or tingling down the leg.
Seek urgent or emergency care right away if you develop:
- loss of bowel or bladder control
- numbness in the groin or saddle area
- major or rapidly worsening leg weakness
These can be warning signs of cauda equina syndrome, which AAOS describes as a surgical emergency.
Common questions about piriformis syndrome exercises
Can piriformis syndrome exercises make symptoms worse?
Yes. They can if you stretch too aggressively, push through pain, or use the wrong movement for the real cause of your symptoms. Stop if symptoms clearly intensify or spread farther down the leg. The NHS advises stopping exercise immediately if you feel pain or become unwell.
Is walking good for piriformis syndrome?
Often, yes. Walking is commonly recommended because it keeps you active without prolonged sitting. Cleveland Clinic lists walking as a preferred cardio option when it does not increase pain.
Should you stretch the piriformis every day?
Some people tolerate gentle daily stretching well, especially in short sessions. What matters more is symptom response than strict frequency. If daily stretching makes symptoms worse, reduce volume and focus more on controlled strengthening and movement breaks.
Are piriformis syndrome and sciatica the same thing?
No. Piriformis syndrome is one possible cause of sciatica-like symptoms, but sciatica can also come from low back problems such as a herniated disk or spinal stenosis. That is why persistent leg pain, numbness, or weakness deserves proper assessment.
How long does it take for exercises to help?
That varies. Cleveland Clinic advises checking with a provider if you are not improving after about a month of consistent stretching and exercise.
Is rest better than exercise?
Usually not complete rest. Cleveland Clinic specifically notes that rest is not the answer for many cases and that a consistent regimen of stretching and exercise can improve symptoms.
Conclusion
Piriformis syndrome exercises may help ease tightness, improve hip mobility, and reduce sciatica-like discomfort when done gently and consistently. Start with a few simple movements, avoid pushing into pain, and get medical advice if symptoms are severe, worsening, or unclear.
